Association between bipolar disorder and diabetic ketoacidosis/hyperosmolar hyperglycemic state
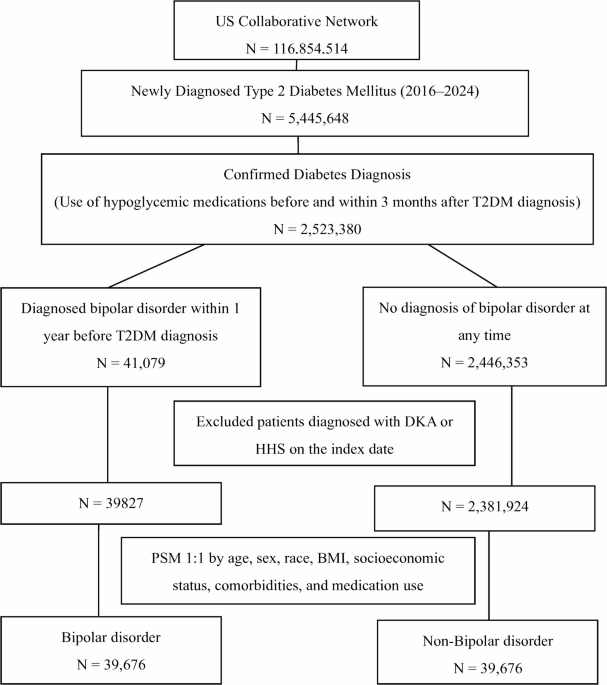
In this large retrospective study of newly diagnosed T2DM, coexisting bipolar disorder was linked to a notably higher risk of acute hyperglycemic crisis (DKA or HHS). Even after propensity score matching for demographics, comorbidities, and medication use, patients with bipolar disorder had a 13% increased hazard of experiencing these events. While prior literature has established that patients with serious mental illness face higher rates of medical complications15, our findings specifically pinpoint DKA and HHS as significant concerns for T2DM patients who also have bipolar disorder.
Furthermore, subgroup analyses revealed several other important associations that warrant further exploration. Notably, younger patients (< 65 years) showed a significantly increased risk. One potential explanation is that younger adults with T2DM may present with a more aggressive disease phenotype and may also be more prone to erratic adherence patterns, including inconsistent follow-up or medication use16. They might also have less stable psychosocial support networks, or a higher prevalence of other risky behaviors, amplifying the impact of bipolar disorder on metabolic control17.
We also observed that White patients had a significantly higher risk of DKA/HHS in the bipolar cohort compared to other racial groups. This finding is somewhat paradoxical, as prior literature consistently reports that non-White populations, particularly Black and Hispanic individuals, have higher risks of hyperglycemic crises and diabetes-related hospitalizations due to structural healthcare disparities, lower access to outpatient care, and socioeconomic factors affecting disease management18,19. Moreover, disparities in referral, treatment adherence, and the recognition of early hyperglycemic symptoms might contribute to racial differences in acute complication rates. Further investigation into these potential mechanisms is warranted.
Interestingly, being married was associated with an elevated risk of hyperglycemic crises in our sample of bipolar T2DM patients. While marriage is often considered a source of social support, it is possible that caregiving responsibilities or stressors arising from family dynamics can complicate the management of both bipolar disorder and T2DM20. Alternatively, married individuals may have different health-seeking patterns that lead to earlier or more frequent diagnoses of DKA/HHS episodes, thus raising observed event rates. Additional qualitative research could help clarify how marital status interacts with mood symptoms and diabetes self-care.
Additionally, our data indicated that patients with a history of cerebrovascular disease faced a markedly higher risk of hyperglycemic crises. Stroke and other cerebrovascular conditions can impair cognition, mobility, and overall capacity for daily self-management6. In bipolar disorder, these challenges might be magnified; periods of mania or depression could further erode adherence to complex therapeutic regimens, increasing susceptibility to acute metabolic decompensation15. Clinicians should be vigilant about reinforcing diabetes education, medication adherence strategies, and routine follow-up for patients with both cerebrovascular disease and bipolar disorder.
In our analysis, Black or African American patients, GLP-1 receptor agonist users, and individuals who were never married or in domestic partnerships exhibited numerically lower risks of hyperglycemic crises, although these findings were not statistically significant. The reduced risk observed among Black patients contrasts with prior literature reporting higher rates of diabetes complications in this population and may reflect detection bias, residual confounding, or variability in EHR documentation21,22. Similarly, GLP-1 receptor agonists are associated with improved glycemic control and reduced glucose variability, which may contribute to lower crisis risk among users23. The inverse association observed with marital status is also notable; while marriage is often considered a source of social support, unmarried individuals may engage differently in self-care or healthcare utilization24. These findings should be interpreted with caution but may offer hypotheses for future investigation into subgroup-specific risks and protective factors in diabetes management.
In our subgroup analysis, Black or African American patients exhibited a lower risk of hyperglycemic crises compared to White patients, which contrasts with prior literature documenting higher rates of diabetes-related complications in this population21. One potential explanation is referral or detection bias: heightened clinical awareness of disparities may prompt more intensive monitoring or earlier intervention in historically underserved groups, thereby reducing the incidence of acute events. Alternatively, this paradox may reflect limitations inherent to electronic health record–based studies, including variability in documentation practices, incomplete coding, and unmeasured confounding.
Finally, the higher risk observed among those with insulin prescriptions likely reflects a subset of patients who had more severe hyperglycemia at T2DM onset or who developed rapid disease progression25. While insulin therapy is essential for many individuals, it also necessitates strict monitoring and consistent dosing—tasks that may become more difficult during mood episodes. This combination of severe baseline hyperglycemia and the self-care complexities posed by bipolar disorder can predispose patients to DKA or HHS if insulin use is disrupted.
Recognizing bipolar disorder as an independent risk factor for hyperglycemic emergencies may prompt tighter integration of diabetes and psychiatric care. Clinicians who treat T2DM in patients with bipolar disorder should consider more frequent glucose monitoring, early dietary and adherence counseling, and close observation for early signs of mania or depression that might interfere with self-care. In psychiatric practice, selecting or adjusting medication regimens with lower metabolic risk—when feasible—could help mitigate excessive weight gain and hyperglycemia, while prophylactic use of metformin or other agents might attenuate medication-induced metabolic problems. In both settings, involving family members or caregivers, when appropriate, could bolster adherence, especially during severe mood episodes.
A major strength of this study is its large and diverse real-world sample, drawn from multiple healthcare systems, which increases the generalizability of results. The robust propensity score matching and thorough adjustments reduce the likelihood of confounding by factors such as age, BMI, comorbid conditions, and baseline medications. Restricting the analysis to newly diagnosed T2DM allowed us to track the emergence of DKA and HHS from an early point. Furthermore, our findings remained consistent across subgroup analyses.
Nonetheless, certain limitations must be considered. First, misclassification is possible in EHR-based studies: some patients labeled as T2DM might actually have latent autoimmune or type 1 diabetes, and bipolar disorder diagnoses depend on accurate clinical coding. We attempted to limit such errors by medication criteria, yet some misclassification is likely. Second, we lacked detailed information on the severity or phase of bipolar illness (e.g., mania vs. depression at diabetes onset), as well as direct measures of medication adherence. Finally, data predominantly reflect U.S. healthcare systems, potentially limiting generalizability to other countries or under-resourced settings with different care patterns.
In this large retrospective cohort study, adults with newly diagnosed T2DM who also have bipolar disorder exhibited a substantially heightened risk of acute hyperglycemic crises—DKA or HHS—compared with matched controls. This association, reflecting both pharmacologic and behavioral factors, underscores the importance of integrated management approaches. Frequent glucose monitoring, proactive education on treatment adherence, vigilant selection and monitoring of psychiatric medications, and collaborative care across mental health and diabetes specialties may help prevent severe metabolic decompensation. Future investigations should focus on targeted interventions and more detailed exploration of mood episodes to develop effective strategies for minimizing DKA/HHS in this susceptible population.
link








