Four people, three female and one male, took part (individual data not reported to avoid identification). Participants had a range of SCI characteristics incomplete/complete; tetraplegia/paraplegia as defined in the ASIA/ISCoS International Standards for Neurological Classification of Spinal Cord Injury (ISNCSCI). Through this collaborative co-design process, the MHM was fittingly modified so that the content was comprehensible, suitable for people’s different circumstances, and maintained a strengths-based orientation while recognising that serious mental health challenges can still arise [15]. Four themes were interpreted to summarise how lived experience improved the MHM. Each theme is described below with illustrative quotes.
Theme one: mental health is front and centre
The first theme described participants’ collective agreement that having a module focusing on mental health was most certainly a non-negotiable necessity for a community self-management resource for people with SCI. This theme was evidenced through various references to mental health being the foundation on which other self-management strategies can be applied. As one participant said: yes the [MH] tool box is good because it allows mental health to sit in front of all other topics [FG001]. In a similar vein, another participant highlighted how addressing mental health can increase the readiness of people to engage in other SCI-HMT topics: because all other [HMT] topics like bladder care for example are further back in one’s mind – compared with mental health [FG004].
Participants reported how having mental health front and centre served to normalise the significant challenge that a SCI presents to a person’s coping resources. Just knowing that many people experience significant mental health challenges was helpful in itself, as one participant reflected: even just saying it’s (mental health) is normal is a great help… I think definitely mention it (mental health) because then someone really will think, oh phew. I’m not abnormal after all [FG004]. Indeed, having a resource that acknowledged how MH challenges are a very real part of the adjustment process following SCI was welcomed by participants. For example, one participant highlighted how following a SCI, people can question whether they have the capacity to go on:
it is really nice and simple and given that a lot of people – maybe most newly injured people – like I did myself – just want to stop living after their injury – I think the toolbox is a sort of relief to read [FG003].
In summary, theme one underscored that mental health was indeed a priority issue. However, participants were quick to remind researchers that it was important to promote the importance of mental health for functioning and wellbeing without overwhelming readers with too much detail.
Theme two: striking the right balance
The second theme describes participants’ desire for the MHM to strike the right balance of acknowledging the serious impact of mental health issues but without undue negativity. For example, while the honest framing of mental health issues was considered positive: “I like it. It is to the point – quite blunt” [FG004], concern was expressed that people with SCI who might read this content may already be feeling ‘vulnerable’ and be susceptible to an overemphasis on negative outcomes. As one participant said: “things like mood fluctuate enormously, especially in the early days – enormous variation in every given day – even an hour” [FG003]. Participants indicated that in the original “academic” draft, the complex language, theoretical constructs, and style placed too much emphasis on the negative aspects of mental health disorders and management, which could detract from its value:
“Well I think it is really useful and might allow people to sort out what the greatest concern is. But you have to be careful that if I wasn’t depressed, I might be after looking at this module.” [FG003]
Participants were quick to emphasise that the toolkit should never be seen as a substitute for professional help. Since deteriorating mental health can have very serious consequences, participants consistently stressed the fine line which exists between trying to self-manage one’s mental health and knowing when (and how) to seek professional support – a decision which can be further clouded by deteriorating mental health. As one participant said,
we can’t take away from the fact that people, like, if they are suicidal, if they are having, like depression and anxiety, they really need to seek professional support. [FG002]
Participants also highlighted that no matter how well a self-management resource may be designed, and what information it may communicate, there is essentially (particularly in serious cases) no substitute for professional support. For example, one participant remarked:
Perhaps that’s when it’s, you refer on to services… because I think that there’s a there’s maybe a, a level of support that that person requires that maybe that the tool won’t be up to address [everything] and help is needed. [FG001]
In summary, theme two described how the MHM needed to strike a delicate balance between highlighting the potential to experience serious mental health issues while not overly stressing the negative aspects of adjustment following and SCI. This can be helped through a positive orientation, which is examined below.
Theme three: the glass is half full
The third theme emphasised the need to for the MHM to focus on positive aspects of the adjustment process. While feedback suggested some negative mental health outcomes need to be mentioned, participants felt several negative adjectives could be removed (for example unhappy, miserable) to reduce the negativity without lessening the seriousness of the message. Participants felt that the information within the MHM could describe both the challenging realities of adjustment, as well as emphasise the positive outcomes implicit in the adjustment process. For example, one participant said:
it not nice to have to go through bladder issues and bowel issues where you know this grief that you’re going through is totally normal (and) through grieving, through process of acceptance, there is light at the end of the tunnel. [FG002].
A more positive framing was achieved through including a simplified description of an evidence-based adjustment model based on the SCIAM [19] (which emphasises the influential role of personal appraisal and the power of a person to direct their mindset and behaviours). The original description was too complex, as one participant said:
the words in the diagram, this SCI adjustment model. There’s a lot of very long words there that could be expressed more simply. [FG004]
In response, the simplified description of the SCIAM was intended to fulfil two key functions: 1) to ensure that the message was understandable to a wide range of potential readers with different levels of health literacy, and 2) emphasising that a person still has control over their adjustment process and outcomes following a SCI. Often this sense of control may not be readily apparent, and may depend on a person’s readiness to change, as one person remarked:
People are only going to access the resource if they are ready to acknowledge that they may be suffering from mental health illness and wanting to change their circumstances to be more informed and improve their mental health [FG002]
In summary, theme three underlined the need to acknowledge that positive outcomes were possible following a SCI, and that the MHM needed to have resources to assist people to understand aspects of adjustment within their control, which were applicable to a variety of people. This leads to our last theme, which highlights the need to create a module which is sensitive to individual circumstances.
Theme four: variety’s the spice of life
The fourth theme highlighted the need for the MHM to be sensitive to individual circumstances and to not imply certain outcomes would inevitably apply to everybody, as one participant said:
“the thing is every person with a spinal cord injury is just that – one person with a spinal cord injury” [FG003]
For this reason, words like ‘will’ were replaced with ‘might’ or ‘can’. For example, If you do not resolve your grief, you will become emotionally drained, at risk of feeling overwhelmed sad, angry and worried was changed to If you do not resolve your grief, you may become emotionally drained, at risk of feeling overwhelmed, sad, angry or worried.
At first glance, this may seem merely semantic tinkering. However, the potential for unintended and implicit negative messages to be passed on through the tone of language cannot be underestimated. For example, while many people do face significant adjustment challenges following SCI – not everyone does. It is easy to assume everyone will be susceptible to the same contributing factors or outcomes, as one participant said:
I wouldn’t generalize to say that everyone that has a spinal cord injury has that [mental health challenges], but obviously there are a lot of people that do, [FG001]
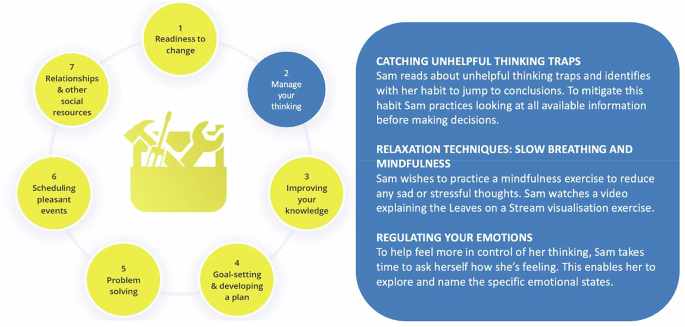
Further efforts to highlight the variety of lived experience were adopted. These included inserting lived experience quotes as examples of positive outcomes, and the addition of several interactive activities in the Toolbox designed to help illustrate how people can develop unique strategies to reflect their circumstances (see Fig. 1 for worked example of somebody using the skills in step 2 of the Toolbox – Manage your thinking).
link